Vulvodynia Explained: Why Vulvar Pain Happens and How to Treat It
Understanding Vulvodynia: What It Is, Why It Happens, and How to Find Relief
Do you ever notice burning or stinging after wearing a pair of leggings that are too tight? Or stood up after a long car ride only to notice a deep soreness near your pelvic floor that felt disproportionate to the situation?
For many women, that discomfort doesn’t just pass. It lingers, returns, and slowly becomes part of daily life, even when there’s no visible irritation, infection, or clear explanation. This chronic vulvar pain is called vulvodynia.
Despite how common it is, vulvodynia is often misunderstood, misdiagnosed, or minimized. In this article, we’ll break it down in clear, practical terms - what it is, why it happens, and what may be driving your symptoms so you can better understand your body and begin taking steps toward real relief.
What actually is “Vulvodynia”?
Vulvodynia is the medical term to define chronic pain or discomfort around the vulva (the external part of the female genitals - see photo below) that lasts for three months or more and often doesn’t have a clear definitive cause.
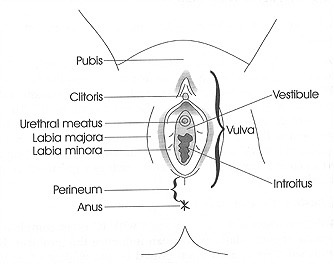
The pain can show up as the following:
· Burning
· Stinging
· Irritation
· Rawness
· Soreness
· Sharp or shooting sensations
Sometimes it affects the entire vulva (generalized vulvodynia), and other times it can be localized to one specific spot, often near the vaginal opening (localized vulvodynia or vestibulodynia).
The vestibule is the urethral and vaginal opening as seen in the photo below.
The pain might be constant or only triggered by touch/pressure. Touch or pressure might be as follows: sitting, when inserting a tampon, wearing tight clothing, wiping after going to the bathroom, or during sexual activity.
Vulvodynia can impact an individual's daily life, intimacy, and emotional well-being.
What Causes Vulvodynia?
There isn’t usually one single cause of this condition. Vulvodynia is multifactorial, meaning it often develops due to a combination of factors. Some of the possible contributors include:
1. Nerve sensitivity
The nerves around the vulva can become overly sensitive, sending pain signals even when there’s no actual injury or inflammation.Sometimes this starts after an infection, irritation, or trauma, but the nerves remain “switched on.”
2. Pelvic floor muscle tension
The muscles that support the pelvic organs can become tightor overactive, leading to pain and tenderness around the vulva. This tension can also make penetration painful.
3. Hormonal changes
Low estrogen levels for example, during menopause, after childbirth, or when using certain birth control pills can cause the vulvar tissues to become thinner, drier, and more sensitive.
4. Past infections or irritation
Yeast infections, urinary tract infections, or reactions to soaps, detergents, fabrics, or scented products can irritate the vulvar tissues and “train” the nerves to remain hypersensitive.
5. Genetic and inflammatory factors
Some women may have genetic differences that make their nerves more reactive or their tissues more prone to inflammation. Vulvodynia is common in people with autoimmune disorders, mast cell activation syndrome, endometriosis, and many other inflammatory conditions.
6. Emotional and psychological factors
While vulvodynia is not caused by anxiety or stress, chronic pain can be worsened by them. Over time, fear of pain or negative pastexperiences can cause the body to hold tension and intensify the discomfort.
How Is Vulvodynia Diagnosed?
Vulvodynia can be tricky to diagnose because it’s a“diagnosis of exclusion,” meaning your healthcare provider needs to rule outother possible causes first.
A typical diagnostic process might include:
· A detailed medical history: Your provider will ask about your symptoms, duration, and possible triggers.
· Physical examination: A gentle exam of the vulva to check for skin changes, tenderness, or areas of pain.
· Cotton swab test: Lightly touching areas of the vulva with a cotton swab helps pinpoint where the pain is located.
· Tests to rule out infections: Swabs or cultures may betaken to exclude yeast, bacterial, or viral infections.
You might also be referred to additional specialists such as a gynecologist, dermatologist, pain specialist or pelvic floor physicaltherapist for further evaluation and collaboration of care.
Treatment Options for Vulvodynia
The encouraging part is that vulvodynia can be treated. It may take a bit of patience and trial and error to find what works best for you,but there are many effective approaches.
1. Lifestyle and self-care adjustments
Small changes can go a long way in reducing irritation:
· Wear 100% cotton underwear and avoid tight clothing.
· Skip perfumed soaps, douches, and scented wipes.
(What is douching? Washing/cleaning the inside of the vagina and rectum with a solution. The vagina is self-cleaning, no vaginal cleansing necessary!)
· Use gentle, hypoallergenic, fragrance-free laundry detergent.
· Try sitting on soft cushions or a donut cushion to reduce pressure.
· Use water-based lubricants during intimacy and avoid lubricants that include scents or aloe.
2. Topical treatments
Your healthcare provider might recommend:
· Topical lidocaine: A numbing gel that can help reduce nerve sensitivity before sexual activity or for daily relief.
· Estrogen/Progesterone creams: Helpful if hormonal changes are contributing to symptoms.
· Other compounded creams: Such as those containing amitriptyline or gabapentin, which calm irritated nerves.
3. Oral medications
Sometimes medications that act on the nervous system can help reduce pain signals. These may include:
· Tricyclic antidepressants (TCAs) like amitriptyline.
· Anticonvulsants like gabapentin or pregabalin.
These medications don’t mean your pain is “psychological”,they’re used to calm the overactive nerve pathways causing the discomfort.Discuss with your doctor if you believe that you are dealing with vulvodynia.
4. Pelvic floor physical therapy
One of the most effective (and empowering!) treatments for vulvodynia involves working with a pelvic floor physical therapist.
Pelvic floor specialists help you:
· Learn to relax and control your pelvic floor muscles.
· Release tension and tightness that may be contributing to pain.
· Gradually retrain your body to tolerate touch and movement again.
· Identify products and strategies to decrease vulvar pain that work specifically for you and your physiology. We know how frustrating(and expensive) it can be to try to treat your symptoms yourself and do your own research. We treat vulvodynia every day! We can assess your specific symptoms and provide a treatment plan tailored to what you need.
Many women notice a big improvement after consistent therapy sessions.
5. Counseling and support
Chronic pain can take a toll emotionally, physically, and sexually. Working with a mental health therapist experienced in chronic pain, trauma, or sexual health can help you navigate those challenges and improve intimacy and confidence.
6. Nerve blocks or surgery (rare)
In severe cases that don’t respond to other treatments, pain specialists may offer nerve blocks or, rarely, surgical options such as a vestibulectomy. These are typically reserved for specific cases and always discussed carefully with your healthcare provider.
Living Well with Vulvodynia
Living with vulvodynia can feel discouraging at times, especially if you’ve seen multiple doctors or been told “everything looks normal.” But progress is absolutely possible. Finding the right care team is important.
Many women find that a combination of treatments like seeing a gynecologist or urogynecologist, pelvic floor therapy, gentle self-care, and targeted medications leads to significant relief over time.
It’s also helpful to connect with others. Support groups(online or local) can provide understanding, encouragement, and practical tips from people who understand.
Resources: National Vulvodynia Association
The Takeaways
If you’re dealing with persistent vulvar pain, know that it’s not your fault and you don’t have to suffer in silence.
If you’re experiencing symptoms of vulvodynia, you can see a pelvic floor physical therapist. They’re trained to understand the complex relationship between your muscles, nerves, and tissues and can help you move toward a life with less pain and more comfort. <3
Sources:
GIRALDI A, KRISTENSEN E, LUNDVALL L, PETERSEN C.Vulvodynia. Definition, diagnosis and treatment Acta Obstetricia et Gynecologica Scandinavica. 2008;87(9):893-901. doi:10.1080/00016340802323321
Goldstein, A. T., Pukall, C. F., Brown, C., Bergeron, S.,Stein, A., & Kellogg-Spadt, S. (2016). Vulvodynia: assessment and treatment. The journal of sexual medicine, 13(4),572-590.
Schlaeger JM, Glayzer JE, Villegas-Downs M, et al.Evaluation and Treatment of Vulvodynia: State of the Science. JMidwifery Womens Health. 2023;68(1):9-34. doi:10.1111/jmwh.13456
Merlino L, Titi L, Pugliese F, et al. Vulvodynia: PainManagement Strategies. Pharmaceuticals (Basel). 2022;15(12):1514.Published 2022 Dec 5. doi:10.3390/ph15121514
Paavonen J, Eschenbach DA. Localized Provoked Vulvodynia-AnIgnored Vulvar Pain Syndrome. Front Cell Infect Microbiol.2021;11:678961. Published 2021 Jun 17. doi:10.3389/fcimb.2021.678961



